August is National Immunization Awareness Month (NIAM)

Immunizations are vital to your health as well as the health of those around you. However, there is a lot of conflicting information swirling around about vaccines. Some of these common misconceptions regarding immunizations are discussed below.
Are immunizations safe?
Yes, every vaccine undergoes extensive testing before being approved for use, and safety data is continuously monitored even after a vaccine is released to the public. Vaccine side effects are almost always minor (such as redness or tenderness in the area the shot was given) and disappear within a couple of days. Serious reactions to vaccines are incredibly rare and the small risk does not outweigh the benefit of preventing dangerous and deadly diseases. For example, vaccines have eradicated smallpox and eliminated wild poliovirus in the United States. There are also immunizations that protect against influenza (flu), tetanus, pertussis (whooping cough), pneumococcal pneumonia, shingles, hepatitis A and B, measles, mumps, rubella, human papillomavirus (HPV), and more.
Prior to the development of vaccines, many rare diseases today were much more common and had deadly consequences. For example, more than 530,000 Americans died from Measles every year prior to a vaccine. Now that number is ~61 over the last 10 years. Worldwide, from 2000-2015, measles vaccinations resulted in a 79 percent drop in measles-related deaths worldwide; preventing an estimated 20.3 million deaths. The image below compares how often people became sick from diseases before vaccines were invented, and how common they are now that vaccines are used to prevent them.
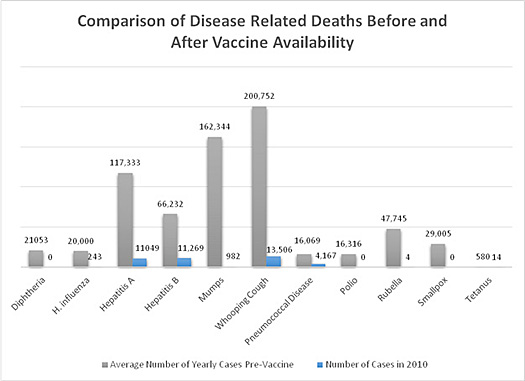
Can children develop autism from vaccines?
There has been no scientific evidence to show that there is a link between vaccinations and the development of autism. Although the cause of autism is poorly understood, both national and international health groups have evaluated that the evidence does not point toward ingredients used in vaccines, such as thimerosal and aluminum, as a cause.
Does everyone receive the same vaccinations?
Not necessarily. People may receive different types of vaccines because of their age or health conditions. Since a child’s immune system continues to develop as they get older, they need to receive some immunizations more frequently than adults. Older adults may also receive different doses of vaccines to protect them against illnesses to which they are more susceptible. One example is the flu shot. Although everyone over six months old is recommended to get the flu shot every year, there’s a high-dose formulation specifically for adults 65 years and older. Those with specific medical conditions such as diabetes, asthma/COPD, HIV, heart, liver or kidney disease, a weakened immune system, or those who smoke may need additional immunizations more often or earlier in life because they’re at higher risk for health complications.
Do some immunizations need to be given more than once?
Yes. One example is the influenza vaccine, which is recommended once every year prior to flu season. There are two reasons for this: one is that your body’s defense against influenza weakens over time. Secondly, the flu virus changes constantly, and each year the formulation of the flu vaccine is reviewed and updated to keep up with the shifting of flu viruses. This means that the flu shot you received last year may not provide adequate protection for this upcoming flu season.
A tetanus booster is needed at least every 10 years. Vaccines that protect against tetanus are combined with vaccines for other diseases; included are Tdap (tetanus, diphtheria, and pertussis) and Td (tetanus and diphtheria). Everyone should receive one Tdap booster in their lifetime and women who are pregnant should receive a dose of Tdap during the third trimester of each pregnancy. It is also important for those who come in close contact with newborns (fathers, grandparents, etc.) to have had a Tdap vaccine to help further protect the baby from developing whooping cough.
Can you get the flu from the influenza vaccine?
You cannot get the flu from the influenza vaccine. The vaccine contains only certain parts of the influenza virus that have been killed. This allows your body to create antibodies to the virus, but your body cannot actually get the flu from the vaccine. Most people who get the flu shot do not have any side effects, but some may experience minor problems such as cough, a mild fever, and headache that may last for one to two days following immunization.
While your body builds up immunity to the flu, which takes up to two weeks, it is possible for you to contract the flu from another source. This is why it is important to get your flu shot prior to the peak of flu season, preferably before the end of October. Even if you don’t get your flu shot by this time, it can still be given throughout the season and provide benefit.
Influenza is the most frequent cause of death from a vaccine-preventable disease and is responsible for 200,000 hospitalizations each year. By getting a flu shot you’re able to create a positive impact for yourself and others. Preventing flu is particularly important for those who are at high risk for complications (very old/young, those with medical conditions, etc.) because they are at higher risk of complications from flu. Some people have conditions that weaken their immune system which prevents them from getting vaccines, so they depend on others to get the vaccine for their protection. It’s also essential to help prevent the spread of illness by practicing good hygiene such as washing hands, sneezing into your arm, staying home when sick, etc.
Why do older people need a shingles vaccine?
The varicella zoster virus causes both chickenpox and shingles, therefore those who have had chickenpox still have the inactive virus inside their body. Our immune system keeps the virus inactive when we’re young, but as we age our immune system begins to weaken, which can cause the reactivation of the virus in the form of shingles. Shingles causes a painful rash, and in some cases the pain can last for months or years after the rash goes away. The shingles vaccine, Zostavax®, is recommended as a one-time vaccination for individuals 60 years and over. The vaccine reduces the risk of developing shingles, and lessens the severity of shingles in those that do develop shingles. If you’ve already had shingles it’s still recommended to be vaccinated to decrease the likelihood and severity of future outbreaks.
What can pharmacists do?
Pharmacists are able to help determine which vaccines are needed and can provide immunizations conveniently at almost any pharmacy location, typically without an appointment. Kelley-Ross has been Seattle’s resource for innovative pharmacy services since 1925. One such service is our partnership with housing organizations to provide immunization clinics. This service provides vaccinations to individuals at their place of residence, making it an easy and convenient way to stay current on immunizations and promote healthy living. Although the service typically focuses on influenza vaccinations during flu season, other immunizations can be provided at the time of service as well.
What can you do?
Talk to your doctor or pharmacist regarding immunizations that you and your family members may need. Increasing the number of people who are vaccinated not only increases an individual’s protection from disease, but also those with compromised immune systems.
If you’d like to find out more information about immunizations, visit the Center for Disease Control and Prevention, Immunization Action Coalition, and the following Kelley-Ross websites—When to get your flu shot, Pneumonia immunizations, and Immunizations offered at Kelley-Ross. In addition, read It’s Never Too Late to Vaccinate in the January 2016 issue of AgeWise King County.
Contributor Katie Mahan, PharmD, is a pharmacy resident with Kelley-Ross Pharmacy Group.
Originally appeared in AgeWise King County (August 2017)
![Aging & Disability Services for Seattle & King County [logo]](https://www.agingkingcounty.org/wp-content/themes/sads/images/seattle-ads-logo.png)